Do you or someone you know suffer from the agonizing wrath of cluster headaches and/or migraines? If so, you’d be part of the stark 52% of our global population annually afflicted by a headache disorder, and 14% of victims suffering from migraines yearly.
With such rampant prevalence, it seems perplexing that up until now, no medications have emerged with 100% efficacy in terminating cluster periods. However, encouraging results on treatment of cluster headaches and migraines with psychedelic compounds like psilocybin and LSD, foretells an optimistic future for those currently under the head-wrenching latch of these disorders.
As you read on, we’ll review and analyze self-recorded, quantitative data on Josh–a Psychedelic Passage survey respondent with chronic cluster headaches who just so happened to have found relief and stability through the use of psilocybin mushrooms. We’ll also be speaking with Dr. Emmanuelle Schindler–a researcher at the Yale School of Medicine who led the first and only controlled study on migraine treatment with psilocybin mushrooms. Before jumping into the innumerable pain and stress-relieving benefits of ‘magic’ mushrooms, a short introduction to the pathophysiology and subjective experiences of these headache disorders is surely warranted.
Cluster headaches (CH), more formally diagnosed as Horton’s syndrome is a severely debilitating disorder that causes bouts or ‘cluster periods’ of recurring attacks in which the affected person experiences harrowing headaches that last about an hour on average and extend over the course of several weeks or months. These cluster cycles then subside for a variable amount of time, sometimes up to a year, in which case the person is considered to be in remission.
Cluster headaches are felt more acutely than migraines, but their individual durations are much shorter. One single migraine may last longer than a CH, but rarely persists for more than a day. In terms of pain allocation, migraine sensations can be confined to specific regions of the head, like behind the eyes, but may sometimes persist throughout the entire cranium- whereas cluster headaches are usually contained to only one hemisphere.
Quite frankly, it’d be difficult to accurately portray the lived experiences of headache disorder victims using only the lens of online news sources and research studies. To properly translate the weight and force of these pains, it’s paramount that the people governed by them also have a say in framing the experience.
We asked a community of migraine-prone people to explain what it’s like to live with this disorder. Here’s what some of them had to say:
“Think about the worst brain freeze you’ve ever had…. Now multiply it by 2, add in a small amount of what feels like an electrical shock, and that splash of pain you get when you dive too deep into the pool…That’s what it feels like to me.”
Warning: this next one is a bit more graphic.
“(It’s like) someone has heated a knitting needle until it’s white-hot and then inserted it into the tear duct of my right eyeball.”
Can ‘Magic’ Mushrooms Really Break the Curse?
I think it’s sufficient to say, stakes are high. Treatment for this very physical and emotional perturbation must find its way into our medicinal pandora box sooner, rather than later. Luckily, traditional medicines like psilocybin mushrooms, cannabis, and even their younger comrade, LSD, have already begun leaving their mark on the symptomatic alleviation of headache disorders. While most ongoing research is still heavily dependent on testimonials from self-medicating individuals, findings are increasingly promising, nonetheless.
We had the chance to speak with Dr. Emmanuelle Schindler from the Department of Neurology at Yale University. Dr. Schindler’s Exploratory Controlled Study of the Migraine-Suppressing Effects of Psilocybin, has pioneered much of what we currently know on the topic. While studying the neuropharmacology of psychedelics during her years at graduate school, she came across reports that suggested their anecdotal effects on headache disorders.
It’s at this point when Dr. Schindler’s initial interest in cluster headaches sparked further curiosity about the potential psychedelics have for treating migraines. Later, in January of 2021, her innovative study would recruit 10 adults suffering from migraines, following them over the course of several weeks. Subjects journaled their symptoms 2 weeks before and 2 weeks after the study to properly compare the effects of this treatment. Results indicated that after a single dose of psilocybin, migraine pain reduced by an average of 1.65 days/week compared to a reduction of 0.15 days/week after consumption of a placebo. Dr. Schindler’s says:
“Migraine is a common headache disorder, so identifying a clinical effect could potentially help a large number of people…. I was pleased that there was preliminary evidence for a clinical effect, though I also knew that much more research would be required.”
The findings of her study are truly encouraging, to say the least. Though psilocybin’s mechanisms of action for treating migraine pain are not yet known, Dr. Schindler tell us:
“This will take me most of my career to uncover. One of the most interesting things is that psychedelics are chemically and pharmacologically similar to conventional migraine medications. Unlike these conventional medications, however, psilocybin appears to have a lasting effect after a single dose; this effect is what distinguishes psychedelics from traditional treatment.”
Dr. Schindler reminds us that further research is, of course, very necessary. While her study gives us evidence for psilocybin’s migraine-relieving effects over the course of 2 weeks, we have yet to examine long term effects in order to understand popper dosing regimens. Dr. Schindler leaves us with this:
“There are ongoing studies in chronic pain disorders, such as cancer-related pain, phantom limb syndrome, and fibromyalgia, so there may be a role for psilocybin and other psychedelics in other pain conditions besides headache. It’ll be important to study each condition separately, however. Psychedelic medicine is not one-size-fits-all; what applies to one patient population does not necessarily apply to another. In addition, psychedelics are not a silver bullet for all human disease; evidence for safety and clinical efficacy will need to be collected for each condition. In order to maintain the new positive reputation of this drug class, I feel this is the best approach.”
Dr. Schindler’s work is evidently commendable and undoubtedly the most well founded evidence we have on the topic. However, we’d also benefit from exploring a qualitative study conducted in 2017 by Martin Andersson et, al. from Karlstad University on treatment of migraines and CH with psychoactive substances, which yielded immensely heartening results.
After narrowing down references abstracted from online discussion forums, researchers indexed overarching empirical themes to establish an accurate consensus on the efficacy of psychedelics in treating these disorders. Reports indicated that self-treatment with LSD and psilocybin significantly reduced the frequency and intensity of CH and migraine attacks. In fact, CH victims very often declared experiences of full remission after only a single dose of these psychoactive medicines. For some ‘cluster heads’, cannabis demonstrated moderate effectiveness in alleviating symptoms, but yielded more variable overall results.
Another qualitative study conducted by Dr. John Halpern from McLean Hospital and colleagues, recruited 53 CH patients. Their research found that 22 out of 26 interview subjects experienced aborted attacks after psilocybin consumption. That’s almost an 85% success rate. 41% of interview subjects experienced less frequent and less intense attacks following use of LSD and psilocybin mushrooms, with a whopping 52% of psilocybin users and 7/8 LSD users reporting complete remission. Moreover, 94.74% of the study’s psilocybin users and 80% of LSD journeyers disclosed a significant increase in the length of their remission period.
As we’ve come to learn, the biological mechanisms underlying psychedelics’ diminishing effects on headache disorders are not well understood. However, some hypothesized influences include psilocybin’s ability to promote neural plasticity, essentially rewiring our brain’s neural network to foster a reorganization of cerebral functions.
Regarding the structure of these compounds, psilocybin’s naturally occurring indole-ring molecules and LSD’s chemically constructed indoles, bind perfectly to serotonin receptor sites. Under the gaze of these substances, increases in dopamine and serotonin (neurotransmitters associated with feelings of happiness and reward) have been documented, and thus are likely to play a vital role in the pain-mitigating effects of psychedelics.
While present legislation limits more widespread studies on psychedelic assisted therapy, that hasn’t stopped Clusterbusters–an organization of fellow ‘cluster head’ activists, from mobilizing efforts to promote psychedelic research for treatment of these disorders. For Bob Wold, founder and president of Clusterbusters, what started as an intrinsic motivation to escape his own quarrels with CH, has now become the nation’s largest non-profit cluster headache organization.
From supporting CH sufferers on an individual scale to aiding massive research developments within the field, Clusterbusters has gained the trust of headache disorder victims and fortified a reputation for offering the most up-to-date information and treatment resources for sufferers of CH. Coming up, we’ll hear a little bit more about the real-life influence of this selfless operation.
A Case Study on Pain, Psilocybin, & Personal Progress
**All parties have consented to the public release of the following information**
As mentioned earlier, much of what we know right now about CH and migraine treatment with psychedelic compounds comes from self-determined research conducted by the very victims of CH. To get a better gauge on the therapeutic experiences of these self-medicating individuals, we spoke to Josh, a long time sufferer of this exhausting condition, who found asylum in psilocybin after countless medicinal trials proved to be futile in relieving his agonizing symptoms.
“Prior to 2015, I used to endure 4-month long cycles, twice per year. From 2015 to 2017 I was chronic. I tried everything from the D3 regimen, to oxygen therapy, sumatriptans and more. Without insurance I spent untold amounts of money. It ruined my livelihood and social life. I felt like I had no control or help and my mental health had significantly deteriorated.”
Blood tests confirmed that Josh’s Vitamin D levels were unusually low, as is common in sufferers of CH. The D3 regimen, aiming to supplement this deficiency, unfortunately only provided Josh with at most, 2 days of relief, before the initial dose became ineffective and he’d find himself constantly needing to up his dosage. Later tests began to reveal a hazardous abundance of D3 in Josh’s blood, this forced Josh to terminate the regimen and left him feeling more isolated and discouraged than ever.
As the story often goes, Josh’s initial encounter with psilocybin rose from typical teenage curiosities, but it wasn’t until 2016 when Josh really hit his breaking point and began to conduct personal research, desperately searching for any ounce of therapeutic hope to treat his CH. Soon, Josh would come to unexpectedly revisit the almost-foreshadowing decisions of his youth.
“I joined a Facebook group for sufferers and saw a post about alternative treatments, including the Vitamin D regimen and psychedelics. From here I stumbled upon a non-profit organization called Cluster Busters where I learned all about psychedelics as a treatment.”
It was now 2017 and Josh was 32 years old, routinely facing up to 5 daily attacks that would persist for nearly 8 hours. At first, fear of catalyzing yet another CH attack made Josh reluctant to explore the mystical realm of psychedelics he’d briefly met in his early 20s. Realizing the extent to which his disorder had percolated stagnation and angst across every facet of his being, Josh made the critical choice to take this leap of faith.
“Close to giving up, I was fortunate to get some psilocybin. A single 1.5g dose busted that 2 year-long cycle, a street value of $10. This was mind-blowing to me. I enjoyed 90 days of remission before a new cycle started. Psilocybin broke that cycle in 90 days and provided me with 16 months remission. The next cycle was only 45 days, followed by 19 months remission. My latest cycle was only 38 days (long). Not only did I experience the positive benefits above, but I track everything, so I can see each cycle includes fewer attacks per week, as well as shorter and less painful attacks in general.”
Now 37 years old, Josh’s forlorn attempts to escape the chokehold of CH, can provide us with real life evidence of psilocybin’s therapeutic benefits. Josh’s proactive decision to document the regression of his CH allows us to quantify the pain-relieving effects of this ceremonious medicine. The following is recent data collected and assembled by Josh over a two month period.
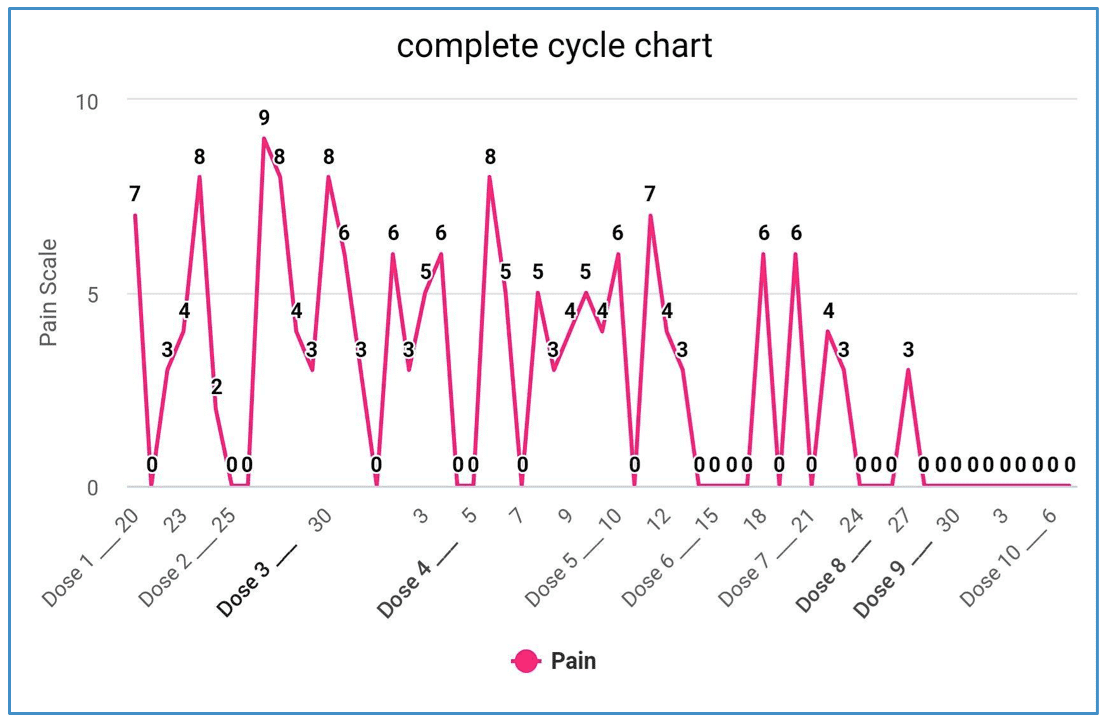
The x-axis of this chart represents days of the month, from March 20th to May 6th and indicates dosing intervals. The y-axis represents his pain scale. This data is consistent with typical microdosing schedules that average 3-5 days in between doses. From his chart we can deduct that at every marked dose, Josh’s CH pain plummets on the scale, climbing slowly over the coming days, then sharply declining following the proceeding dose. Overtime, we see that Josh’s average pain has been consistently decreasing.
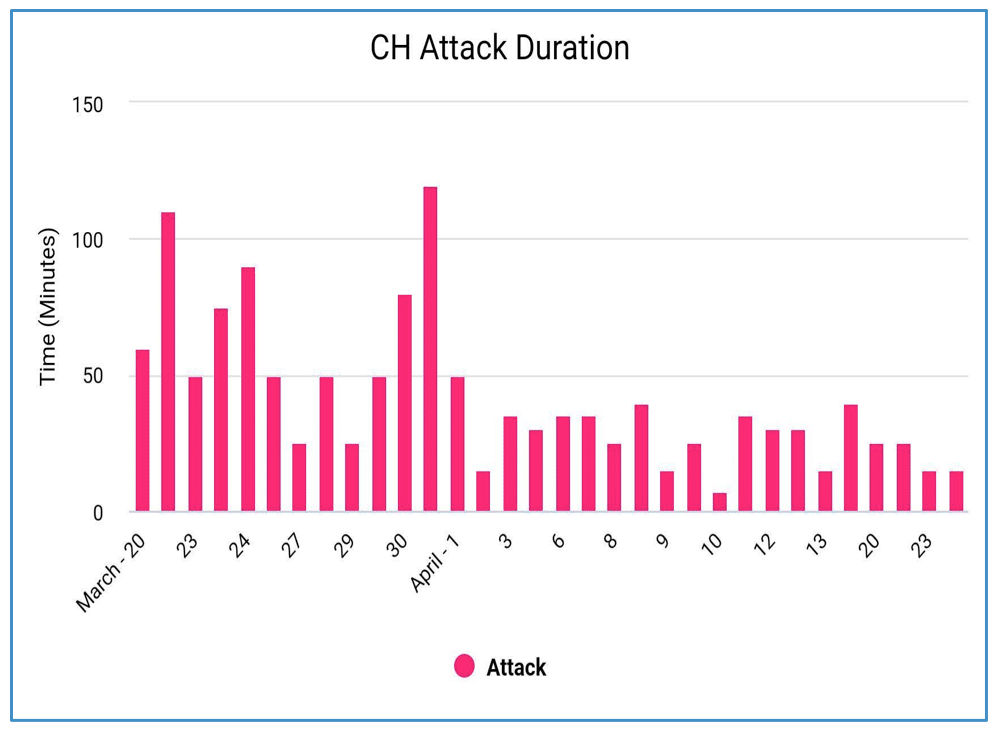
These astounding results support the countless testimonies of headache disorder victims around the globe who’ve turned to psychedelics for ceasing the relentless dudgeon of CH and migraine symptoms. Following his first dose, Josh experienced only 24 hours of being pain-free and 2 doses later, the duration of his attacks plummeted significantly.
Today, he’s able to regard a CH cycle as ‘terminated’ after only 10 days of being pain free! Josh reminds us that for him, the biggest lifestyle differences didn’t come from the reduction of his former pain. Instead, he feels the most significant benefits lie in his relief from the uncertainty of not knowing when an attack will ensue–an anxiety that through time, has come to destroy many of Josh’s professional and social relationships.
“Once an attack begins, not knowing how bad it will get, or (how) long it will last is also devastating overtime, on par with torture. It ruins your livelihood and destroys your mental health. Since 2017, that has all significantly changed for me. I’m optimistic about the pain levels and attack duration. I feel like I have complete control over my life again and that’s been the biggest factor for me.”
Josh generously shared with us the typical dosages that have led to his rapid recovery. He began by taking 1.5 grams of psilocybin and now takes 2.5 grams for maintenance dosing. Though, it should be noted that Josh’s body has a difficult time processing psilocybin which in turn, causes him to consume above average maintenance dose sizes to compensate for his body’s atypical absorption rate.
We’ve actually written an article on this somewhat common phenomenon–why some may not trip (even with high doses). Please take into consideration that dosage size and frequency can greatly vary from person to person, most often dependent on weight/ body mass. That’s why we highly recommend taking these substances under the guidance of an experienced facilitator.
And while you’re at it, give our detailed guidelines a quick read, to learn more about safe and accurate dosing. Next up, we’ll cover your legal choices for taking advantage of these primitive, cutting-edge medicines in a safe and supportive environment.
Relief & Recovery: Starting Your Journey
By now, you must be wondering how exactly one can reap the miraculous headache-relieving benefits of psychedelics. Well friends, here’s where it can get a little tricky. As of right now, clinical trials are the most straight-forward way to partake in ongoing psychedelic research for treatment of CH.
However, rigorous guidelines for participant sample sizes greatly limit public access to these treatments. Depending on where you live, legislation may also prohibit psychedelic research from being conducted, but don’t fret–we’ve actually written an article entirely dedicated to helping you find a psychedelic guide near you. If you find comfort in exploring this experience within a medical setting, reaching out to psychotherapists in your area who are well versed in the nature of these substances, could be your best choice.
Others, though, may be motivated to embark on this journey from the comfort of their own homes. If that resonates with you, we encourage you to have a chat with one of our knowledgeable facilitators. At Psychedelic Passage we offer 1-on-1 ceremonial trip-sitting experiences with specialized programs designed to ensure that anyone and everyone from all walks of life have equal access to the life-changing contributions of psychedelic medicines.
We understand the challenges of traversing such uncharted territory in isolation, which is why our offerings prioritize personal autonomy every step of the way, making certain that your psychedelic journey is focused and curated to your unique, individual needs. Our intuitive psychedelic facilitators are located in every major U.S. city, equipped with the internal abundance to hold a receptive space that embraces your intentions and later, aids in integrating the fruits of your experience.
Whoever you choose to accompany you on this journey, it’s of utmost importance that you advocate for a tripsitter that echoes your own strum of beliefs and devotions to healing. If you want to dig a little deeper into the therapeutic benefits of psychedelic experiences, schedule a consultation with us to get personalized information on all things psychedelic.
One last message before you depart–to our human sisters and brothers under the callous reign of these tyrannical headache disorders–please keep your hopes alive. As our Western society’s approach to modern-day therapeutics continues to draw inspiration from ancient indigenous medicines and practices, we will undoubtedly live on witnessing these exponentially thinning gaps within our current healthcare models. There’s much hope to be held in the ever expanding applications of psychedelic medicines. For now, take care, our fellow cluster heads. May relief and clarity rain upon you.



