Explore the intricate dynamics between antidepressants and psychedelics, particularly focusing on the blunting effects of SSRIs and antidepressants on psychedelic experiences.
We offer an in-depth analysis of serotonergic medication interactions, emphasizing the potential reduction in psychedelic potency and discussing strategies for mitigating these interactions through careful tapering and alternative therapies like microdosing.
Serotonergic medications like SSRIs have been on the market for treatment of mental health conditions like depression and anxiety for several decades now, and they’ve maintained a steady public backing since their conception.
More recently though, the cultural discussion surrounding these regimens has addressed a wide-reaching dissatisfaction with their often intolerable side effects.
It’s this longing for more deep-rooted and durable antidepressant and integrative mental health treatments that have given our psychedelic renaissance such impassioned communal reinforcement.
To the best of our knowledge, this may be the most comprehensive analysis and review to date on the chemico-biological interactions of these medicines in each of their respective drug classes.
We explore the mechanisms by which antidepressants can reduce or amplify the potency of a psychedelic trip and the safety-first steps you can take to reduce negative interactions.
Whether you’re looking to replace a current medication with psilocybin therapy or seeking to combine traditional talk therapy with psychedelic therapy, this discussion on the psychedelic drug interactions will undoubtedly inform your next steps.
Explore more topics like this one in The Encyclopedia of Psilocybin Mushrooms: From Cultivation to Therapy.
Download Our Free Psilocybin Sourcing Guide
For harm-reduction purposes, we provide links to online psilocybin vendors, local stores, delivery services, and spore vendors for growing your own medicine at home.
Key Takeaways
- The current consensus suggests a period of 4-6 weeks following the tapering off of SSRIs to ensure optimal results.
- The Horowitz-Taylor method is often cited as the most effective hyperbolic taper methodology to successfully taper off of SSRI/SNRIs.
- Irrespective of the blunted psychedelic experience there may still be positive neurocompensatory changes that occur as a result of the psilocybin psychedelic, e.g. neuroplasticity, neurogenesis, synaptogenesis.
- Psychedelic Passage: Your Psychedelic Concierge — The easy, legal way to find trustworthy psilocybin guides, facilitators and psychedelic assisted therapy near you in the United States.
Antidepressants That Interact With Psychedelic Medicine
Selective serotonin reuptake inhibitors (SSRIs)
- Citalopram (Celexa)
- Escitalopram (Lexapro)
- Fluoxetine (Prozac)
- Fluvoxamine (Luvox)
- Fluvoxamine CR (Luvox CR)
- Paroxetine (Paxil)
- Paroxetine CR (Paxil CR)
- Sertraline (Zoloft)
Serotonin-norepinephrine reuptake inhibitors (SNRIs)
- Desvenlafaxine (Pristiq)
- Duloxetine (Cymbalta)
- Venlafaxine (Effexor)
- Venlafaxine XR (Effexor XR)
- Milnacipran (Savella)
- Levomilnacipran (Fetzima)
Serotonin partial agonist/reuptake inhibitor (SPARIs)
- Vilazodone (Viibryd)
- Vortioxetine (Trintellix)
Tricyclic antidepressants (TCAs)
- Amitriptyline (Elavil)
- Desipramine (Norpramin)
- Doxepin (Sinequan)
- Imipramine (Tofranil)
- Nortriptyline (Pamelor)
- Amoxapine
- Clomipramine (Anafranil)
- Maprotiline (Ludiomil)
- Trimipramine (Surmontil)
- Protriptyline (Vivactil)
Monoamine oxidase inhibitors (MAOIs)
- Phenelzine (Nardil)
- Selegiline (Emsam)
- Tranylcypromine (Marplan)
- Isocarboxazid (Parnate)
- Moclobemide
Norepinephrine-dopamine reuptake inhibitors (NDRIs)
- Bupropion (Wellbutrin, Aplenzin)
Atypical agents
- Mirtazapine (Remeron)
- Nefazodone (Serzone)
- Trazodone (Desyrel, Oleptro)
- Buspirone (Buspar)
Expectation Management for the Psychedelic Trip
Assuming well informed expectations for psilocybin therapy is key for having an experience that’s tailored to your body’s metabolic needs and to your present mental health conditions.
While some studies on the matter have yielded contradicting findings, a substantial number of anecdotal reports draw a significant, negative correlation between prolonged use of serotonergic medications and the degree to which a psychedelic trip can be inwardly experienced.
“I am on 200mg of Sertraline and took 3.5gs of shrooms last night. It basically felt the same as the first time I smoked pot. Got the munchies, but no hallucinations unless I closed my eyes, and even then there was hardly anything.” –Reddit User
“I take Zoloft and can NOT trip on shrooms. I’ve tried a few times. I think the Zoloft blocks the trip” –Reddit User
In other words, people who are prescribed these pharmaceutical drugs and take them routinely, have reported experiencing little to no hallucinogenic effects on a standard dose of tryptamines, like psilocybin mushrooms and LSD.
Though this phenomena seems to expand its presence into a plethora of other psychedelic drugs, like Phenethylamines (MDMA, mescaline), today we’ll be settling our attention on the trip-suppressing effects of antidepressant pharmaceuticals.
Let’s begin by discussing the mechanisms that scientists believe are encouraging this mind-body discord.
Please note that the infancy of the psychedelic medicine industry unfortunately limits the range of controlled research studies and clinical trials that have investigated less-discussed, sometimes case-specific nuances of our highly variant body of psychedelics.
Though that’s caused most of our current research to rely largely on anecdotal reports, it’s important to recognize the high and widespread frequency of these discouraging interactions.
For the purpose of offering a comprehensive analysis, we’ll be piecing together the findings of several observational studies, to paint a more conclusive scientific explanation for this absorption-related dysfunction.
Current Research Studies on Antidepressants and Psychedelics
In a 1999 study, researchers deduced that the perceptual distortions experienced from hallucinogenic drugs are mainly hosted by 5-HT2A (serotonin) receptors through glutamatergic transmissions occurring in the cerebral cortex (Aghajanian & Malek).
Substances like LSD and psilocybin are bicyclicly structured into an indole-shaped ring. This form allows them to perfectly attach themselves to our brain’s 5-HT2A (serotonin) receptors.
Picture this as the communion of a particular key with its corresponding lock, like the perfect piece to a complex puzzle. It’s worth noting that due to the large molecular size of LSD, it can frequently lead to the 5HT2A receptor becoming “stuck.”
This phenomenon often clarifies why LSD experiences sometimes adhere to a lengthy yet foreseeable sequence, while other times the psychedelic effects can endure well past their expected duration. Now that we understand a small part of psilocybin’s cerebral route, let’s take a look at the mechanisms of antidepressants.
A 2017 study conducted by Carhart-Harris and colleagues investigated the biological mechanisms of antidepressants, particularly their impact on serotonin receptors. According to research published in a study by Amargos-Bosch et al., the primary mechanism of action for antidepressants is through the 5-HT1A receptor system.
They primarily enhance resilience, tolerance, and may induce emotional blunting through this system. Additionally, there is some involvement with the 5-HT2A receptor system, which contributes to their competitive antagonism with psychedelics.
However, the reduced effects observed with psychedelics could also stem from the downregulation of serotonin receptors resulting from long-term, chronic use of SSRIs.
What does this mean? Well, first and foremost, it tells us that compounds like LSD and psilocybin target the same receptors as antidepressants.
It also suggests a conflict of chemical interest, where two drugs are attempting to act on serotonin receptors to alter brain function.
While psilocybin is trying to bind to and activate 5-HT2A receptors (in order to elicit hallucinogenic effects), antidepressants are attaching themselves to these same receptors, then blocking the sites to prevent further 5-HTR binding.
This obstructs our body’s biological response to psychedelic drugs that act on 5-HT2AR, since their serotonin chemicals cannot be freely binded to or stimulated by the clogged receptor.
Essentially, antidepressants inhibit nerve cells from reabsorbing serotonin, thereby increasing the extracellular concentrations of serotonin. Originally, this was believed to induce more “pleasure” in people who were depressed. However, it was later found that stimulation of the 5HT1A receptors allows for the passive coping of stress, both internal and external.
By hindering reabsorption, our brains are given a larger supply of unoccupied serotonin to amplify transmission between its neurons.
A large number of studies hypothesize that down-regulation and desensitization of the receptors is the culprit of our brain’s inability to respond to serotonin, after prolonged antidepressant use. One 2013 study produced findings that supported this notion (Gray et al.).
The study recruited 19 unmedicated subjects with major depressive disorder and compared the binding function of their 5-HT receptors before and after a 5-9 week period of self medication with SSRIs.
Results showed an 18% downregulation of binding functions to 5-HT autoreceptors, congruous with previously conducted animal studies.
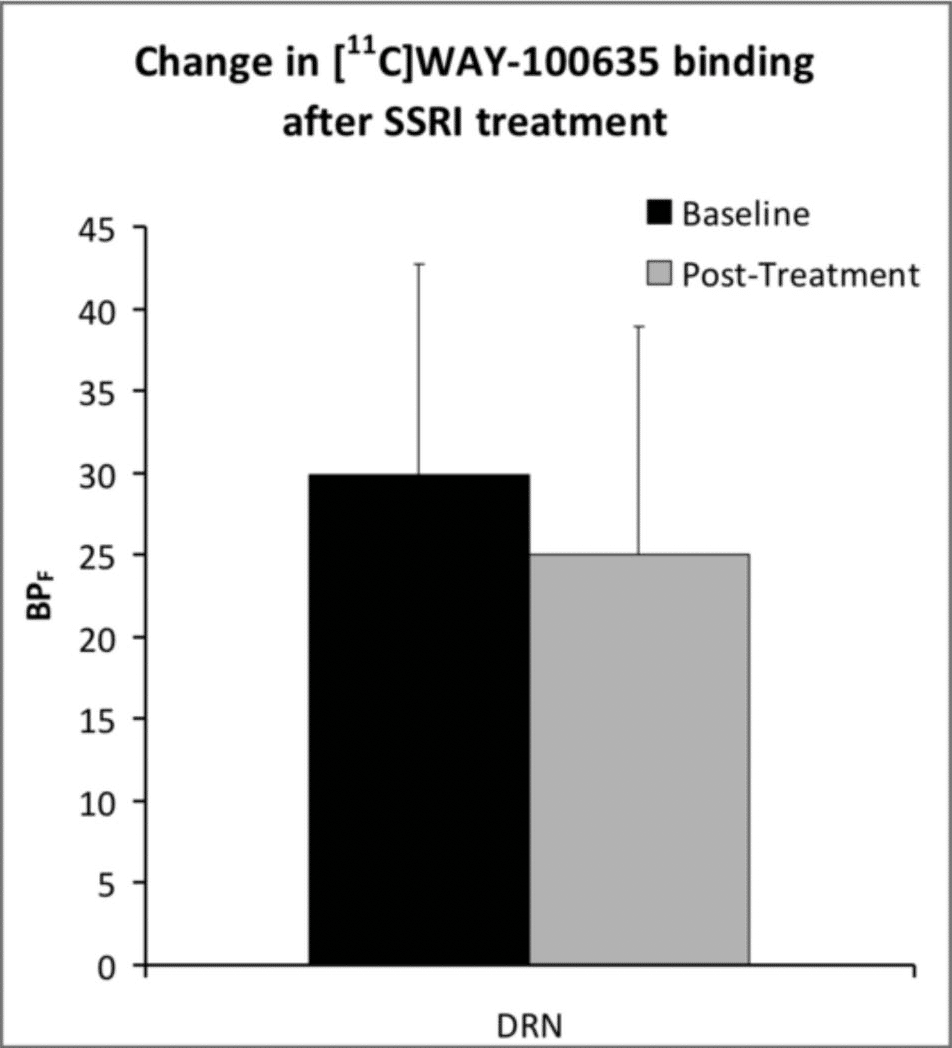
This initial reduction is thought to increase the firing rate of serotonergic neurons in later stages of treatment, magnifying this communication by releasing more serotonin.
However, post-treatment results indicate that this surge is not durably maintained without the antidepressant, and instead it causes our brains to have more trouble producing serotonin than it did pre-treatment.
So the big question–how does these findings communicate the brain’s inability to experience normal levels of psychedelic hallucinations, during and after antidepressant use?
Psilocybin, or more precisely psilocin, shares structural similarities with serotonin (5-HT), differing only by the hydroxyl group being on the 4-position rather than the 5, and the dimethyl groups on the nitrogen. It is psilocin that binds to the 5HT2A receptor as a partial agonist.
Put simply, antidepressants impede the stimulation of the 5HT2A receptor through competitive binding and long-term desensitization and down-regulation of receptors.
Since 5HT receptors are believed to be the primary cause of psychedelic effects, the inhibition of serotonin reuptake means a diminished ability to experience the psychoactive properties of this fungus.
Also, someone who’s only recently stopped prolonged use of antidepressants, may not feel a standard psychedelic dose as potently as someone who’s never been on a serotonergic medication.
Of the very few observational studies directly investigating this phenomenon, a 1996 study recruited 32 volunteers to report on the intensity of their psychedelic experiences while on heavy use of antidepressants (fluoxetine, paroxetine, sertraline, trazodone) (Bronson et al.).
88% experienced a significant reduction of LSD effects after more than 3 weeks of antidepressant dosing.
A 2017 study agreed with these findings, coming to the conclusion that antidepressants evoke 5HT2AR downregulation, consequently blunting the effects of psychedelic drugs (Carhart-Harris & Nutt).
One of their earlier studies examined the effects of tricyclic antidepressants on the LSD experience. After seeking out 10 subjects who had been on TCAs or MAOIs for at least 3 weeks, they gathered their reports on the LSD experience.
A standardized questionnaire revealed a significant correlation between chronic use of TCAs and amplified hallucinatory distortions on LSD. Conversely, participants on MAOIs experienced a significant reduction of subjective LSD effects.
However, another 2017 study came to a much different conclusion. This study found that MAOIs increased the accumulation of 5-MeO-DMT in the central nervous system and enhanced its interaction with 5-HT2A receptors (Halberstadt).
This indicates that MAOIs amplify the effects of 5-MeO-DMT and other tryptamine hallucinogens, rather than diminishing them. It’s important to note that the risk of serotonin syndrome significantly escalates with the presence of MAOIs. MonoAmine Oxidase Inhibitors (MAOI) hinder the breakdown of serotonin, leading to potentially dangerous interactions.
The most perilous combination involves SSRI + MAOI + MDMA, which triggers serotonin release via the SERT pathway. Ayahuasca, a brew containing DMT and an MAOI, underscores why antidepressants are strongly contraindicated with this medicine. Mixing antidepressants with MAOIs can artificially and drastically elevate serotonin levels, posing a severe risk of life-threatening serotonin syndrome
We should note though, the study primarily focused on the alteration of the pharmacodynamics of 5-MeO-DMT by MAOIs and did not directly investigate the subjective effects of the combination of MAOIs and tryptamine hallucinogens in humans.
A 2016 literary review by PK Gillman also concluded that MAOIs should not be taken with drugs intended to release serotonin as their interaction could potentially cause serotonin syndrome—a bodily reaction caused by an excessive amount of amassed serotonin, which could be fatal.
He also agreed that this combination could reduce the effects of psychedelics like MDMA.
Anecdotally, we’re seeing that chronic use of irreversible and non-selective MAOIs can diminish responses to serotonergic psychedelics. Acute use of reversible MAOIS (e.g. harmala alkaloids) can potentiate responses.
To be clear, it is widely believed that combining psychedelics with any drug that inhibits serotonin reuptake will increase the chances of serotonin syndrome, also known as serotonin toxicity. However, this is very unlikely.
Serotonin syndrome, a potentially serious condition caused by excessive serotonin levels, typically results from the simultaneous use of medications that affect serotonin levels, such as SSRIs or SNRIs, and substances that inhibit serotonin breakdown, such as MAOIs.
While classic psychedelics like psilocybin generally do not lead to excess serotonin secretion, substances like MDMA, which promote both serotonin release and reuptake inhibition, pose a greater risk. Understanding these mechanisms is crucial in assessing the risk of serotonin toxicity when combining drugs.
Buspirone’s blunting effects on psychedelics are not caused by inhibition of reuptake, but by their partial agonist properties that may compete with the psychedelic attempts to enter those same serotonin receptors.
A 2016 study by Pokorny and colleagues used a double blind, within-subject design to analyze the effects of Buspirone on psilocybin hallucinations.
The placebo group was given a small dose of ergotamine, an anti-migraine medication, to compare interactions against larger, regular doses of Buspirone.
The Altered State of Consciousness rating scale was used to detail the subjects’ experiences which produced very strong evidence (p<0.001) for a significant decrease in visual hallucinations and a significant decrease in derealisation and depersonalisation (p=0.062), compared to main scale scores.
Ergotamine did not produce any suppressing effects. These results conclude that Buspirone inhibits hallucinatory effects of psychedelic drugs.
To those who’ve found themselves in this colorless situation, unable to experience the therapeutic effects of psychedelic medicine for many different conditions–never fear.
There are steps we can take to ensure our bodies respond to psilocybin as best they can.
Restoring The Serotonin System After Antidepressant Use
A 2019 study by Kathryn G. Commons and colleagues suggests that autoreceptor desensitization isn’t an effect of antidepressants.
They argue against the hypothesis that long term use of antidepressant medications overstimulates serotonin receptors and permanently reduces their ability to continue emitting this autoinhibitory feedback.
Their research suggests that although desensitization may occur, the unaffected receptors do continue inhibiting reuptake, returning our brain to baseline levels of serotonin production using the compensatory feedback inhibitors that remain.
These findings illustrate a positive outcome that seems in line with many of our client’s experiences: After tapering off antidepressants, the brain’s serotonin system returns close-enough to baseline for journeyers to feel the effects of psychedelic medicine.
However, the best available evidence says that there should be about a 4-6 week washout after tapering off of an SSRI. Even then, a 2023 study in the Journal of Psychopharmacology showed that the attenuation of psilocybin mushroom effects can last up to 3 months.

What Have We Seen Anecdotally With Our Clients?
As a company who facilitates psychedelic journeys professionally, we’ve worked with both clients who are on antidepressants and those who are not.
Our take is that antidepressants don’t pose a safety concern when combined with psilocybin treatment, but they do tend to interfere with client expectations.
Chances are if you’re exploring an intentional psychedelic experience, you’re seeking some sort of change.
The challenge is this—what happens if you put all the time, energy, and money towards preparing for a psychedelic experience only to have nothing happen?
For most people, the answer is disappointment. This is why we typically discourage combining serotonergic medications with psilocybin.
The interesting thing is that we’ve had clients send us this study from 2021 which shows the SSRIs don’t interfere with the psychedelic experience—but we’ve found that doesn’t hold true–at least not with all medications.
While the study is a great data point, it’s also important to consider the results we’ve seen anecdotally working with clients first-hand over the last several years.
We’ve sat with clients who are concurrently taking SSRIs and attempting psychedelic experiences. Alternatively, we’ve sat with clients who are taking SSRIs who eat 10+ grams of mushrooms and experience no effects at all.
It’s widely acknowledged that there’s typically a 60-80% reduction in psychedelic activity when SSRIs are in use. This attenuation effect can persist for the first 4-6 weeks after tapering off SSRIs and sometimes up to 3 months.
Although some individuals may report no reduction in psychedelic effects despite SSRI use, they represent a minority. In some cases, higher doses of psilocybin may facilitate a psychedelic state, while others may have a positive albeit incomplete experience.
Recent literature supports these observations, with a growing number of papers documenting positive reports among individuals on SSRIs. Notably, a study indicated worse outcomes in individuals who tapered off SSRIs compared to those who never initiated SSRI treatment.
References:
So, it’s not that the 2021 study is ‘wrong’—just that it doesn’t paint the full picture.
At this point in time, we don’t have enough information to accurately predict whether a client will have a significant psychedelic experience while taking SSRIs–while some may indeed experience such effects, a greater proportion may encounter reduced, absent, or attenuated responses.
Working closely with clients in distress, we’ve learned that managing hope requires careful framing and discussion. Transparency, thorough preparation, and patience can pave the way for a more informed and fulfilling experience, grounded in appropriate expectations.
The question is, is that a risk you’re willing to take as a journeyer? Only you know the answer to that question.
How Long Do I Need to Discontinue Use?
Understanding what should be naturally expected from our body’s present conditions is step number one. Conscious and safe preparation for the psychedelic experience in step number two for ensuring you preserve your physical and mental health.
Before diving into some relevant and effective options for getting the most out of your magic mushrooms, please be advised that cessation of any medical treatment like antidepressants, should always be discussed with your psychiatrist beforehand.
Antidepressant dosage reduction or termination should always be done under the supervised care and direction of a medical professional and should never be abruptly withdrawn.
Abrupt discontinuation of antidepressant medications can worsen mental health conditions and cause emotional instability and volatility.
Having said that, we understand it can be intimidating to approach your doctor with psychedelic-related concerns. If you need some guidance, check out our article on how to speak with your doctor about psilocybin therapy.
However, it’s important to acknowledge that not all psychiatrists possess comprehensive knowledge about psychedelic medicine or tapering protocols for SSRIs. Many, if not the majority, lack expertise in these areas, as they are not typically covered in medical school curriculums or standard residency programs, except for a select few progressive institutions.
In such cases, patients are encouraged to inquire about the credentials that qualify their psychiatrist as an expert in advising on topics like psychedelics.
Now, let’s review what can be done to promote better absorption of psilocybin to hopefully yield more adequately-weighted therapeutic psychedelic effects.
Traditional Tapering Method vs. The Horowitz-Taylor Method
The Horowitz-Taylor method is a tapering approach that’s frequently praised for its effectiveness in safely discontinuing the use of SSRI/SNRIs (Selective Serotonin Reuptake Inhibitors/Serotonin-Norepinephrine Reuptake Inhibitors). These medications are commonly prescribed for conditions like depression and anxiety.
Traditionally, the American Psychiatric Association (APA) recommended relatively quick tapers over a period of up to 2 weeks. However, this rapid tapering often results in severe withdrawal symptoms that patients find difficult to tolerate.
To mitigate withdrawal effects, experts typically advise tapering to at least 3 times the medication’s half-life. The half-life is the time it takes for half of the drug to be eliminated from the body. However, many successful tapering regimens extend over a much longer period, often 10 weeks or more.
The tapering process may vary depending on factors such as the duration of medication use and the dosage. For instance, if someone has just started taking the medication or is on a very low dose, a faster taper may be feasible. However, it’s essential to recognize that psychotropic medications exhibit a hyperbolic binding pattern, which means that even small doses can have significant effects on receptor binding.
Therefore, reducing the smallest doses can be particularly challenging because they represent a disproportionately larger amount of receptor binding. This underscores the importance of careful, gradual tapering to minimize withdrawal symptoms and ensure a successful discontinuation of SSRI/SNRI medications.
- If you’re taking any of the SSRIs or SNRIs referenced in the first chart, including SPARI drugs like Vilazodone (Viibryd) or Vortioxetine (Trintellix), with the exception of fluoxetine, consider tapering off of your medications to 3 times the half-life of the medication.
- If you’re on fluoxetine, discontinuation of medication should occur at least 6 weeks prior to your journey. By the time you’re ready to embark on the trip, you should have ceased consumption of any SSRI drug.
- While Wellbutrin typically does not diminish traditional psychedelics, it’s worth noting that it can still affect their potency. Wellbutrin should not be combined with Ayahuasca. Additionally, it has been observed to increase the effects of MDMA.
- On a Mirtazapine medication, tapering should also allow for a 2 week period of discontinued use, prior to your trip. Mirtazapine could dull psychedelic experiences, similar to SSRIs and SNRIs, but its blunting mechanisms lie in a blockage of the 5HT2A receptor, rather than blocking the 5HT reuptake pump.
- This same 2 week tapering regimen should be applied for those on Tricyclic antidepressants. Discontinuation before a psychedelic trip is advised due to the potential for experiencing intensified psychedelic effects and serotonin syndrome.
- If on Trazodone, tapering and discontinuation should be in effect a minimum of 5 days before a trip to prevent blunting effects.
- Buspirone consumers should also follow the 5-day minimum to avoid the same events.
- MAOIs should be discontinued through tapering 2 weeks before a trip for these same reasons.
- The combination of Lithium and psilocybin appears to pose potential risks, as it may lead to toxicity and increase the likelihood of adverse outcomes such as seizures, serotonin toxicity, or negative experiences.
How Microdosing & Psychotropic Medication Can Help
Microdosing psilocybin mushrooms may potentially be helpful for those looking to taper off of psychotropic medications such as antidepressants, anti-anxiety medications, stimulants, antipsychotics, and mood stabilizers.
This is because psilocybin binds to the 5-HT receptors which are linked to mood, social behavior, sexual desire, memory, sleep, appetite and digestion among many other things.
The theory behind including microdoses of psilocybin while tapering off pharmaceuticals is largely based on anecdotal reports. As of now, there is no research evidence supporting this theory.
The idea suggests that microdosing psilocybin may act as a natural supplement to the systems influenced by psychotropic medications. Proponents of this theory propose that such supplementation might potentially lessen or even eliminate pharmaceutical withdrawal side effects altogether, such as brain zaps, fatigue, and irritability.”
Many people report feeling lighter and more alive while taking microdoses with their psychotropic medications, even while tapering.
The other benefit to microdosing during the tapering process is that it increases neuroplasticity in the brain (Ly et al., 2018). Although microdosing effects are sub-perceptual, they allow for the brain to form and reorganize synaptic connections.
In other words, a microdosing protocol allows the brain to be re-wired in a way such that it is not dependent on pharmaceutical medications.
In summary, microdosing psilocybin potentially allows one to taper off of their psychotropic medications faster and with far fewer withdrawal side effects.
Important Note: Because many psychotropic medications also work through the serotonin pathways, it will sometimes require a higher dose of psilocybin for the effects to be felt. This is normal, simply adjust your dosage as necessary.
However, recent research suggests that individuals using psilocybin alongside SSRIs may experience positive outcomes, potentially due to cellular changes such as neurogenesis, neuroplasticity, and synaptogenesis.
However, the exact mechanisms are not yet fully understood. Therefore, adjusting your psilocybin dosage as necessary is recommended, while remaining mindful of potential interactions with other medications.
How to Determine Your Psychedelic Dose
Until recently, assessing the potency of psychedelic substances required sending samples to a lab, a costly and time-consuming process. However, recent advancements have led to the availability of at-home testing kits, including ones for mushroom material.
These at-home kits, like QTests by Miraculix, not only confirm substance presence but also provide precise measurements of potency, either in milligrams or as a percentage. This enables users to accurately dose and tailor their experiences, crucial for avoiding overwhelming or underwhelming effects.
Understanding potency is essential for therapeutic use, as different doses can result in vastly different experiences. For microdosing, it ensures consistent daily doses.
Qtests offers:
QTests provide a scientifically validated method for determining the concentration of unregulated substances, granting both journeyers greater control over treatment processes and safeguarding the potential benefits of psychedelic therapies.
Explore Harm Reduction Products:
- The Best Purity Test Kits for Psychedelic Therapy
- How to Test The Potency of Psychedelics At Home: Mushrooms, LSD, MDMA
- The Best Mushroom Grow Kits for Psychedelic Therapy
- The Best Spore Vendors for Psychedelic Therapy
Helpful Tips For Tapering Off of Antidepressants
The best way to taper off, adjust, or eliminate any medication is with the supervision and guidance of your prescribing doctor or psychiatrist.
However, we also recognize that many doctors are better at prescribing medications than they are at helping people taper.
This often results in them recommending tapering regimens that are far too aggressive and lead to significant withdrawal symptoms.
For most people, these withdrawal symptoms are so disruptive and debilitating that it seems easier to continue to use a particular pharmaceutical drug in order to avoid the return of depressive symptoms.
In an effort to provide you with some general guidelines, we’ve outlined a tapering protocol established by Adele Framer, the founder of survivingantidepressants.org:
Since 2011, Surviving Antidepressants has advocated a conservative 10% reduction per month of the most recent dose – an exponential taper, the size of each reduction becoming progressively smaller, approximating the hyperbolic method endorsed by recent research (Framer, 2021).
These gradual tapers to minimize withdrawal symptoms typically require the creation of customized dosages and take many months to several years, depending on individual tolerance for dosage reduction.
Why reductions at monthly intervals? Although diagnostic criteria require withdrawal to appear within a week of dosage reduction, our members report it can take several weeks (or more) for them to appear.
People may not recognize incipient symptoms themselves or it may take some time for symptoms to culminate. Pharmacokinetically, enough residual drug may be active to forestall withdrawal symptoms through the washout period.
If the taper proceeds without significant problems, for most drugs, people generally reduce to less than 2.5% of the original dosage before stopping completely.
Given the potential lag time in emergence of withdrawal side effects, the person should be monitored for at least 3 months after discontinuation, with low-dose reinstatement at the ready should subsequent withdrawal symptoms appear.
To reiterate, taper slowly and listen to your body at all times. It is common for withdrawal side effects to have a delayed onset up to 2 weeks.
Oftentimes a more conservative tapering process will be faster in the long run than forcing things and ending up in the start/stop cycle.
What About Medications Other Than Antidepressants?
Stimulant medications like Adderall and Vyvanse have a much shorter half life. Prescription stimulants may not affect the psychedelic experience noticeably, but microdosing may be a useful alternative. For more information, check out “Can You Mix Psychedelic Mushrooms With Adderall and Stimulants?“.
The procedure for using psychedelics if you’re on opioids may be dependent on the specific medication you’re on. However, a medication like Wellbutrin (Bupropion) is a non-issue in combination with serotonergic psychedelics.
Bupropion primarily affects the norepinephrine and dopamine systems, with minimal direct impact on serotonin. Psilocin, on the other hand, primarily affects serotonin receptors. This suggests that the two drugs have different primary mechanisms of action and do not directly interact at the receptor level.
Additionally, Bupropion is metabolized in the liver, primarily by CYP2B6, to its active metabolites. Psilocin is metabolized from psilocybin through a different pathway. Therefore, there is no known direct interaction between these metabolic pathways.
Atypical antipsychotics (e.g. chlorpromazine, risperidone, ketanserin) appear non-toxic but diminish responses to serotonergic psychedelics.
Typical antipsychotics (e.g. haloperidol) appear to increase risks of anxious ego-dissolution and dysphoric experience.
Buspirone appears non-toxic but may compete with psilocin or downregulate serotonin receptors to diminish responses.
When it comes to other psychotropic medications, we suggest speaking with our team of psychedelic concierges to ensure that all potential contraindications are accounted for.
Drugs like benzodiazepines should never be tapered off without consulting a medical professional. The withdrawal symptoms of benzodiazepines can be life threatening and should not be taken lightly.
Helpful Resources
- Should I Stop Using Antidepressants for Psychedelic Therapy?
- Top 5 Ways to Consume Psychedelic Mushrooms for Therapy
- How Often Should You Take Psilocybin Mushrooms?
- How Long Should You Microdose Psychedelic Mushrooms For?
- The Psychedelic Therapy Process: A Step-by-Step Guide
Our Services & How We Support Your Psychedelic Journey
Psychedelic Passage is dedicated to supporting your psychedelic journey through providing access to safety resources and psychedelic facilitation services.
We believe in the transformative potential of psychedelics when approached with the right knowledge, guidance, and preparation. Our commitment is centered on providing access to accurate and comprehensive information about these medicines.
We offer you access to a network of pre-vetted professional psychedelic facilitators who are experienced and well-trained, specializing in guiding individuals through their psychedelic experiences in a safe and supportive manner.
They play a crucial role in ensuring a positive and enriching journey by providing guidance on contraindications, proper dosing, and general preparation.
On the day of your psychedelic journey, our facilitators are there to offer continuous support, creating a nurturing and comfortable environment for your experience.
Overall, our organization strives to empower and support individuals on their psychedelic journey, offering a holistic approach that includes education, guidance, preparation, day-of support, and integration assistance.
Get Matched with a Trusted Psychedelic Therapy Provider Near You
Hi there! We sincerely hope that you’ve found valuable takeaways that resonate with your current intentions. To explore research-based education, stay updated with psychedelic news, and benefit from practical how-to articles, we encourage you to head over to our resources page.
If you’re seeking personalized advice and are prepared to take the first step toward a therapeutic psychedelic experience, we invite you to book a consultation with our team of experienced psychedelic concierges.
This consultation is more than just a conversation; it’s an opportunity to be matched with a trustworthy local facilitator. You’ll be seamlessly connected to our rigorously vetted network of psychedelic guides, ensuring potential matches align with your needs.
Psychedelic Passage offers confidence and peace of mind by alleviating the burden of having to guess who’s right for you. If you want to discover how Psychedelic Passage can help you, we empower you to learn more about our services and check out client testimonials from those who’ve gone before you.
Your healing path is uniquely yours, and our commitment is to serve you at every juncture. Psychedelic Passage: Your Psychedelic Concierge — The easy, legal way to find trustworthy psilocybin guides, facilitators and psychedelic assisted therapy near you in the United States.
Learn More About Our Network
- Meet Our Referral Network
- Explore Frequently Asked Questions
- Watch Client Testimonials
- Book a Consultation Call
- Is Psychedelic Passage Safe & Legit?
Frequently Asked Questions: Antidepressants & Psychedelics
Q: Can I take antidepressants and psychedelics together?
It’s generally advised to avoid combining antidepressants with psychedelics due to potential interactions. Antidepressants, especially SSRIs, can diminish or alter the effects of psychedelics, making the experience unpredictable and potentially less effective.
Aside from psychedelics being blunted by antidepressants, combining the two could potentially increase the risk for serotonin syndrome, so it’s best to taper off prior to ingesting psychedelics.
Q: Can psychedelics be used as an alternative to traditional antidepressant medications?
Psychedelics—specifically psilocybin—have been shown in recent studies to be an effective antidepressant and even treatment method for treatment-resistant depression.
However, they are not currently approved as a standard alternative to traditional antidepressants given the complex legality around these substances.
Q: How might psychedelics affect my mental health if I have a history of depression?
Because depression is a complex condition, there is no guarantee that taking a psychedelic will have a reliable effect (but then again, even prescribed medications have the same issue).
Overall, many studies suggest potential therapeutic benefits for depression, but in cases of extreme mental health issues, consulting a professional and having a great deal of support is pertinent if experimenting with these medicines.
Connect With Psychedelic Passage
- Listen to our podcast on Spotify, Apple Podcasts, and iHeartRadio
- Subscribe to our Youtube Channel
- Follow us on Instagram, Reddit, Twitter, and Linked in for bite-sized updates and content.
References:
- Aghajanian, G. K., & Marek, G. J. (1999). Serotonin and hallucinogens. Neuropsychopharmacology, 21(2 Suppl), 16S-23S. https://doi.org/10.1016/S0893-133X(98)00135-3
- Amargós-Bosch, M., Bortolozzi, A., Puig, M. V., Serrats, J., Adell, A., Celada, P., … & Artigas, F. (2004). Co-expression and in vivo interaction of serotonin1A and serotonin2A receptors in pyramidal neurons of prefrontal cortex. Cerebral Cortex, 14(3), 281-299. https://doi.org/10.1093/cercor/bhg128
- DL;, B. K. J. (n.d.). Chronic administration of serotonergic antidepressants attenuates the subjective effects of LSD in humans. Neuropsychopharmacology : official publication of the American College of Neuropsychopharmacology. https://pubmed.ncbi.nlm.nih.gov/8726753/
- Bonson, K. R., Buckholtz, J. W., & Murphy, D. L. (1996). Chronic administration of serotonergic antidepressants attenuates the subjective effects of LSD in humans. Neuropsychopharmacology, 14(6), 425-436. https://doi.org/10.1016/0893-133X(95)00145-4
- Serotonin and brain function: A tale of two receptors – RL carhart-harris, DJ Nutt, 2017. (n.d.). https://journals.sagepub.com/doi/full/10.1177/0269881117725915
- A review concerning dietary tyramine and drug … (n.d.-a). https://www.psychotropical.com/wp-content/uploads/2017/12/MAOI_diet_drug_interactions_2016.pdf
- Pokorny, T., Preller, K. H., Kraehenmann, R., & Vollenweider, F. X. (2016). Modulatory effect of the 5-HT1A agonist buspirone and the mixed non-hallucinogenic 5-HT1A/2A agonist ergotamine on psilocybin-induced psychedelic experience. European Neuropsychopharmacology, 26(4), 756-766. https://doi.org/10.1016/j.euroneuro.2016.01.005
- Commons, K. G., & Linnros, S. E. (2019, July 17). Delayed antidepressant efficacy and the desensitization hypothesis. ACS chemical neuroscience. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC7340170/
- Ly, C., Greb, A. C., Cameron, L. P., Wong, J. M., Barragan, E. V., Wilson, P. C., Burbach, K. F., Soltanzadeh Zarandi, S., Sood, A., Paddy, M. R., Duim, W. C., Dennis, M. Y., McAllister, A. K., Ori-McKenney, K. M., Gray, J. A., & Olson, D. E. (2018, June 12). Psychedelics promote structural and functional neural plasticity. Cell reports. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC6082376/
- What I have learnt from helping thousands of people taper off antidepressants and other psychotropic medications – Adele Framer, 2021. (n.d.). https://journals.sagepub.com/doi/full/10.1177/2045125321991274
Becker, A. M., Klaiber, A., Holze, F., Istampoulouoglou, I., Duthaler, U., Varghese, N., Eckert, A., & Liechti, M. E. (2023, February 14). Ketanserin reverses the acute response to LSD in a randomized, double-blind, placebo-controlled, crossover study in healthy participants. The international journal of neuropsychopharmacology. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC9926053/#:~:text=LSD%20potentially%20could%20be%20trapped,making%20its%20downstream%20effects%20irreversible
Erritzoe D;Barba T;Spriggs MJ;Rosas FE;Nutt DJ;Carhart-Harris R; (n.d.). Effects of discontinuation of serotonergic antidepressants prior to psilocybin therapy versus escitalopram for major depression. Journal of psychopharmacology (Oxford, England). https://pubmed.ncbi.nlm.nih.gov/38520045/
Goodwin GM;Croal M;Feifel D;Kelly JR;Marwood L;Mistry S;O’Keane V;Peck SK;Simmons H;Sisa C;Stansfield SC;Tsai J;Williams S;Malievskaia E; (n.d.). Psilocybin for treatment resistant depression in patients taking a concomitant SSRI medication. Neuropsychopharmacology : official publication of the American College of Neuropsychopharmacology. https://pubmed.ncbi.nlm.nih.gov/37443386/
Gukasyan, N., Griffiths, R. R., Yaden, D. B., Antoine, D. G., & Nayak, S. M. (n.d.). Attenuation of psilocybin mushroom effects during and after … https://journals.sagepub.com/doi/10.1177/02698811231179910
Serotonin and brain function: A tale of two receptors – RL carhart-harris, DJ Nutt, 2017. (n.d.). https://journals.sagepub.com/doi/full/10.1177/0269881117725915
van Os, J., & Groot, P. C. (2023, May 9). Outcomes of hyperbolic tapering of antidepressants. Therapeutic advances in psychopharmacology. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC10185864/#:~:text=The%20Horowitz%2DTaylor%20method%20for,lower%20than%20registered%20dosages%20are

Dr. John Moos, MD
Dr. John Moos is a former Trauma and Acute Care Surgeon with over two decades of experience across several hospitals, including Sutter Health Memorial Medical Center and North Valley Hospital District. He earned his medical degree from the University of California, Davis School of Medicine, followed by postgraduate training at Keck School of Medicine at USC, where he served as Chief Resident in General Surgery.
Transitioning from trauma surgeon to trauma healer, John felt called to put the scalpel down. He embraced holistic healing practices and founded Soul Surgeon MD, a psychedelic healing sanctuary in Los Angeles. As a member of the Psychedelic Medicine Association and The American Society of Ketamine Physicians, Psychotherapists, and Practitioners, he now focuses on integrating psychedelic therapies into his unique healing framework.




